🦀 PT Crab Issue 116 - You Are Vital. Please Take Vitals.
This week we’re talking about vitals and why PTs don’t take them, how they should take them, and one crazy case where vitals really pointed the diagnosis the right direction. That’s for our King Crab members (thanks y’all!) they get triple the amount of articles per week and the warm fuzzy feelings from supporting this independent project. And more. You can become one by clicking the link here: https://ptcrab.org/subscribe. Thanks!
For y’all free subscribers, you get one piece all about how to take vitals correctly because #vitalsAreVital
With that, let’s dive in!
How to Take BP Correctly
The Gist - This excellent piece from the Journal of Cardiopulmonary PT is a detailed assessment of how to properly take PT. According to them, “Hypertension is the most common primary diagnosis in the United States. It is a major risk factor for coronary heart disease, stroke, and renal failure, and affects 29% of the adult US population. Twenty-two percent of persons who have hypertension are unaware that they have it.” And PTs see people so often that we’re in a great place to help monitor this. But inaccurate measures of BP aren’t helpful, especially since the paper points out that many people are borderline: “almost two-thirds of hypertensive individuals would be denied morbidity preventing treatment if the diastolic blood pressure were underestimated by 5 mm Hg; the number of persons diagnosed with hypertension would more than double if systolic pressure were over estimated by 5 mm Hg.“
So how do we do it well? Buckle up.
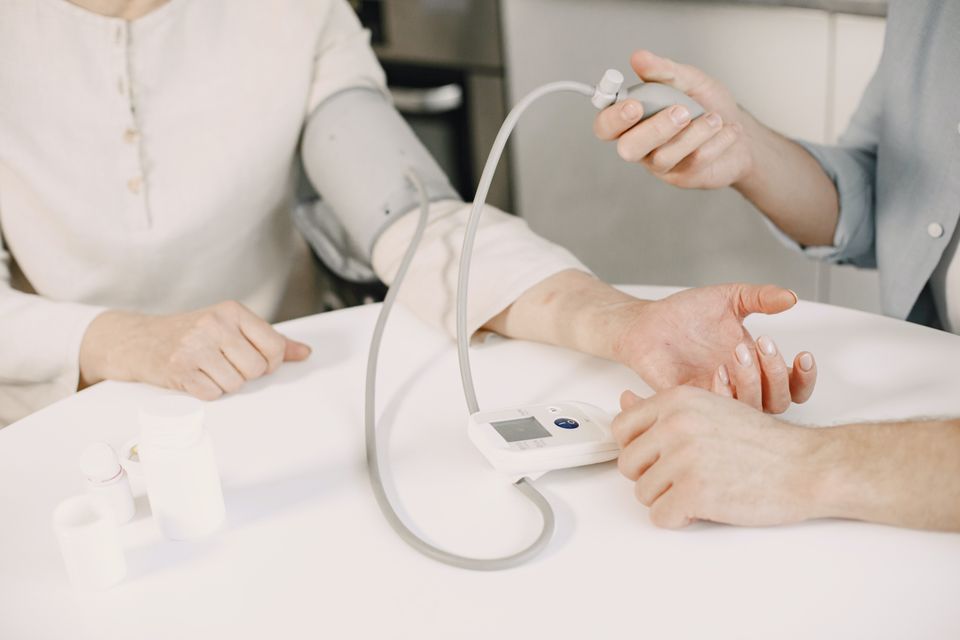
The blood pressure cuff should be placed on the patient’s bare arm. If necessary, clothing should be removed, and the patient/client draped, to adequately expose the arm. The sleeve should not simply be rolled up in order to gain access to the arm; it creates a tourniquet effect above the cuff. When placing the cuff on the arm, the midline of the inflatable bladder should be positioned over the brachial artery…at the mid-point of the upper arm. The lower-most edge of the cuff should be at least 1 inch (2.5 cm) above the antecubital crease so that the bell (preferred) or the diaphragm of the stethoscope can be placed over the point of the strongest palpable brachial artery pulse in the antecubital fossa without encroaching beneath the cuff….
Because of the effects of hydrostatic pressure, the position of the arm when the blood pressure is measured can also have a major impact on the pressure observed. The magnitude of this effect is 1 to 2 mm Hg for every 2.5 cm above or below the level of the heart… since muscle contraction raises blood pressure, care should also be taken to avoid the patient/client helping to elevate the limb; if available, pillows or bolsters may also be used to properly position and support the arm.
In order to avoid over inflation of the cuff, and to accommodate any systolic auscultatory gap, the clinician should estimate a maximum inflation point by palpating the radial pulse while incrementally inflating the cuff until the pulse disappears. The therapist should then wait at least one minute after deflating the cuff before reinflating the cuff to 30 mm Hg above the point where the pulse previously disappeared.
Tell Me More - They have a few more things to watch out for. I think we all know that crossing legs increases BP by about 5mmHg, so uncross those things. And forearm BPs are unvalidated and can differ up to 20mmHg from upper arm, so watch out for those too.
They also recommend that standing BP be performed in the elderly after performing seated to watch out for postural hypotension. That’s a systolic BP drop by more than 20mmHg or diastolic by more than 10mmHg.
Lastly, picking the correct size of cuff is key. Too small leads to overmeasuring, and too big is better but causes errors in both directions. Also, those automatic cuffs aren’t actually very accurate and quite suspect, according to the paper, so do it by hand and do it quick, ideally twice to verify.
Paper? Got it here. And it’s open access.
And that’s our week! Thanks for tuning in and please share with friends, family, colleagues, the lot. Thanks!
Here’s this week’s bibliography:
- Frese, E. M., Fick, A., & Sadowsky, H. S. (2011). Blood pressure measurement guidelines for physical therapists. Cardiopulmonary physical therapy journal, 22(2), 5–12. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3104931/


Comments
Want to leave a comment and discuss this with your fellow PTs? Join PT Crab and get summarized PT research in your inbox, every week.