PT Crab 🦀 Issue 137 - So, you fucked cancer.

If you are or are well acquainted with a cancer survivor, you’ll know that things don’t end when the cancer is gone. That’s just the beginning of a new phase. That phase expresses itself in many ways, but the way we’re talking today is exercise.
There are 15.5 million cancer survivors in the United States, a figure that our first paper expects to double in the next few decades. Even as a student, I worked with dozens of cancer survivors and I’m sure you work with them in clinic all the time. So today, we’re going to look into exercise recommendations for cancer survivors in our first paper and a review of safety considerations in cancer rehab in our second. Just two papers for King Crab supporters today, as these summaries are going to be long. Thanks for your support!
With that, let’s dive in!
P.S. Special thanks to Dr. Elise Kantu, AKA TheOncoPT and Dr. Nicole Stout, renowned cancer researchers and PTs, who both helped make recommendations for this edition of the Crab.
How to Exercise After Cancer
The Gist - This 2018 roundtable of cancer experts came together in San Francisco, sitting down 40 experts from 20 countries to hash out evidence-based exercise prescriptions for folks after cancer. They did a fantastic job with this piece. I’m not going to go through the methodology any more to say that it was well done. The finished product sorts the health effects of exercise based on how much evidence we have about them. They also have some great tables of specific recommendations at the end. I can’t go through all those tables, but if you regularly work with cancer survivors there are breakdowns of how to exercise people for specific conditions, e.g. for lymphedema, there aren’t specific recommendations for aerobic exercise (there are for most conditions), they recommend resistance exercise at 60-70% of 1RM with 1-3 sets of 8-15 reps 2-3x/wk, and there aren’t recommendations of aerobic + resistance (there are for most conditions here too). So let’s talk specifics.
There was strong evidence that exercise is effective for improving:
- Anxiety
- Depressive symptoms
- Fatigue
- Health-related Quality of Life
- Lymphedema
- Physical Function
Moderate evidence that exercise is effective for improving:
- Bone health
- Sleep
And insufficient evidence that exercise is effective for improving:
- Cardiotoxicity
- Chemotherapy-induced neuropathy
- Cognitive function
- Falls
- Nausea
- Pain
- Sexual function
- Treatment tolerance
Tell Me More - To dive into the strong ones:
Anxiety - “Moderate intensity aerobic training three times per week for 12 weeks or twice weekly combined aerobic plus resistance training for 6–12 weeks can significantly reduce anxiety in cancer survivors during and after treatment.” But resistance training alone doesn’t reduce anxiety. The effect is stronger in supervised programs as well.
Depressive symptoms - “Moderate intensity aerobic training performed three times per week and for at least 12 weeks or twice weekly combined aerobic plus resistance training lasting 6–12 weeks can significantly reduce depressive symptoms in cancer survivors during and after treatment.” Like with anxiety, resistance training alone doesn’t seem to be effective. It looks like there’s a dose-response relationship, where higher volumes lead to better symptom control.
Fatigue - “For training programs that last at least 12 weeks, engaging in moderate intensity aerobic training three times per week can significantly reduce cancer-related fatigue both during and after treatment. Moderate intensity combined aerobic plus resistance training sessions performed 2–3 times per week or twice weekly moderate intensity resistance training may also be effective, and the latter particularly in prostate cancer.” Their results showed that low intensity exercise was unlikely to reduce fatigue and that >150 minutes per week did not appear to reduce fatigue more than shorter programs.
Health-related Quality of Life - “Combined moderate intensity aerobic and resistance exercise performed 2–3 times per week for at least 12 weeks results in improvements in HRQoL both during and after treatment. The benefit of combined aerobic plus resistance training programs appears more potent than programs consisting of only aerobic or resistance training.”
Lymphedema - “For resistance training, a general progressive program focused on large muscle groups performed 2–3 times per week, with the principle of ‘start low, progress slow’ is safe when supervised by a fitness professional.” Keep an eye out though, as “Insufficient evidence exists to conclude whether or not starting a resistance training program without supervised instruction is safe for women with or at risk for lymphedema after breast cancer.” So we just don’t know yet, it’s probably safer to start supervised. A clinic I did a rotation at actually had a special program designed just for this! And people seemed to like it pretty well.
Physical function - “Moderate intensity aerobic training, resistance training or combined aerobic plus resistance training performed three times weekly for 8–12 weeks can significantly improve self-reported physical function.” This result is unsurprising, but hey, we gots to study the things. Like the others, supervised exercise tends to work better, but not a ton better.
For the other categories, the moderate evidence ones, you’ll have to check out the whole paper. The specific recommendations in a table are there as well, that’s Table 2. But my favorite part is box 3, because it’s so efficiently laid out:
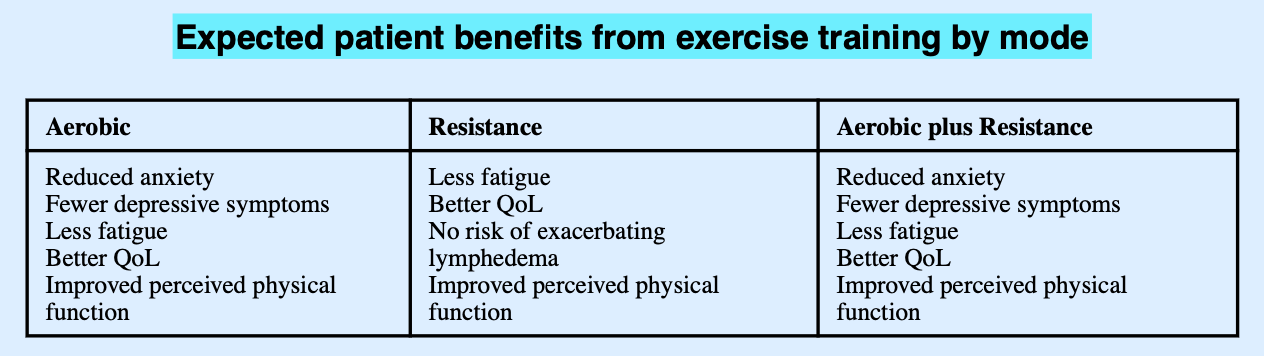

For more like that, do check out the excellent, open access paper. Maybe print it out or save it to refer to in future? It’s a good idea.
Paper? Gotcha.
Brought to you by Hint Water
If you're like most PTs I know, you probably don't drink enough throughout the day. But it doesn't have to be that way.
Water doesn't have to be boring!
Hint Water specializes in flavored water infused with fruit essences. Unlike sweetened beverages or artificially flavored drinks, Hint Water offers a refreshing and tasty alternative without the addition of sugar or diet sweeteners. By using purified water and natural fruit essences, Hint Water provides surprisingly accurate fruit flavors. We offer 8 delicious flavors to choose from.
Try Hint Today! New customers get over 45% off your first order + FREE Shipping and support PT Crab in the process. Click here for your deal and use promo code SwapStack
But what about safety?
The Gist - This focused review of safety considerations in cancer rehab was authored in part by Dr. Nicole Stout who is a dynamo in this field. If you’re going to follow the research of one person about cancer rehab, I’d say she’s the one.
This article is much more complex than the previous, though shorter, which is nice. Let’s look into some common concerns that come up with almost everyone who has had cancer at first, then we’ll look into some more specifics below.
- Post-surgical precautions and contraindications are common in cancer rehab and it’s important for clinicians to be aware of what’s going on, while balancing those concerns with the importance of post-operative mobility.
- Chemotherapeutic interventions come with a big mix of side effects, much too big to get into here, but there’s a fantastic table of them organized by both category and name, along with side effects. I’ll put a picture below to show how nice this table is. If I worked in cancer rehab, I’d have this printed out or saved on my desktop.
- Anemia “is a frequent complication of cancer and cancer treatment including chemotherapy and radiation” and it reduces exercise tolerance and endurance. They recommend that caution be used “ in prescribing progressive resistive and moderate to high intensity aerobic exercise in individuals with severe anemia (hemoglobin ≤8 g/dL). And that you monitor hemodynamic, functional, and exertion status
- Thrombocytopenia is something to watch out for too. “Individuals with platelet counts below 10,000 k cells/uL are at significant risk for spontaneous hemorrhage” while people with 20,000 or less are restricted to walking and ADLs. You need more than 30,000 k cell/uL to be safe for moderate exercise.
All of the above is specifically important in folks undergoing bone marrow transplantation. Exercise helps these folks recover and shortens the duration of anemia, neutropenia, thrombocytopenia, and hospitalization length, but it’s gotta be done safely.
Tell Me More - This is a big paper. The next sections concern cardiopulmonary toxicity, neurotoxicity, lymphedema, frailty, osseous fragility, cachexia, and more. We’re obviously not going to get into all of that. I’m going to pull out some highlights, then get into specific safety considerations about exercise.
Some notes:
- “One of the most commonly used chemotherapy drug classes, anthracyclines, may have significant and irreversible impact on cardiac function, primarily resulting in reduce left ventricular function. Over time, this reduces overall ejection fraction and compromises long term cardiac function.”
- Chest wall radiation can adversely impact both cardiac and pulmonary function. This type of radiation is common with breast, lung, and Hodgkin’s cancer treatments and can result in diastolic dysfunction and blood flow abnormalities.
- Platinum-based chemotherapeutic agents can have a “persistent impact on sensation and proprioception are notable and are shown to have a negative impact on balance, gait, and mobility even > 5 years after the completion of treatment.” Because of this, “fall risk is two to three times greater in the population of individuals with a history of receiving neurotoxic chemotherapeutic agents.”
- Exercise does not exacerbate lymphedema or have significant impact on worsening symptoms. Additionally, “there is no strong evidence basis for the use of compression garments during exercise for prophylactic purposes, however early use of compression therapy in the presence of early, sub-clinical lymphedema is safe and effective.” And watch for cellulitis.
- If cachexia and sarcopenia aren’t treated properly, exercise can actually make them worse, since they need appropriate protein and energy balance.
There’s a lot more, but let’s look into exercise specifically. If you’re interested in modalities, Table 5 in the paper breaks down contraindications in cancer survivors. But notes about exercise for the most common cancers, breast and prostate, are below:
“Exercise training and maximal and sub-maximal exercise testing in persons with breast cancer is relatively safe. However, because 35–58% of breast cancer survivors report persistent shoulder and arm pain, it is important to minimize the risk of musculoskeletal injuries which may result from surgical intervention or hormonal therapies.”
“Greater than 50% of individuals undergoing prostate cancer treatment will receive androgen deprivation therapy (ADT) to alter hormonal impact on tumor growth. ADT is associated with muscle mass depletion and bone density loss which directly impact safety with rehabilitation interventions. Aerobic and resistive exercise interventions mitigate the impact of ADT and promote restoration of muscle mass and mitigate bone density loss.”
Exercise also appears to be safe in people experience leukemia, though watch out for blood associated stuff from above.
Overall, the paper is specific to point out that physical therapy rehabilitation is generally safe in oncology patients as long as we keep safety considerations in mind.
Check out the paper for more details.
Paper? Ye ye ye.
And that’s our week! Thanks for reading along and inviting friends, as usual. This one was intense on the topic, I know. Next week we’re talking flat feet, then neck pain after. Stay tuned for more!
Cheers,
Luke


Comments
Want to leave a comment and discuss this with your fellow PTs? Join PT Crab and get summarized PT research in your inbox, every week.