🦀 PT Crab Issue 65 - Stop being an expert
This week in PT Crab, we’ve reverted a bit by presenting a paper that deals with our outpatient ortho sweet spot, but one that doesn’t as well. We’re looking into practice patterns around IASTM (and they’re very diverse) and how to stop being an expert and start being a coach (and why). Our King Crab supporters got two more articles this week, one on what manual muscle testing of the different trap areas are actually testing, and a second that’s a consensus statement (plus a beautiful website) about physical activity for people with long term conditions. Subscribe to that and get all the supporter perks here.
Also this week, PT Crab has been featured on the Healthy, Wealthy, and Smart podcast, a show for PTs by a PT who talks to all kinds of people about how to make your life and practice better. That episode drops next week, here are some of their episodes in the meantime to tide you over.
- 245: Dr. David Butler: Explain Pain Supercharged
- 378: Mick Hughes & Randall Cooper: Melbourne ACL Rehabilitation Guide 2.0
Now, let’s dive in!
How to stop being an expert.
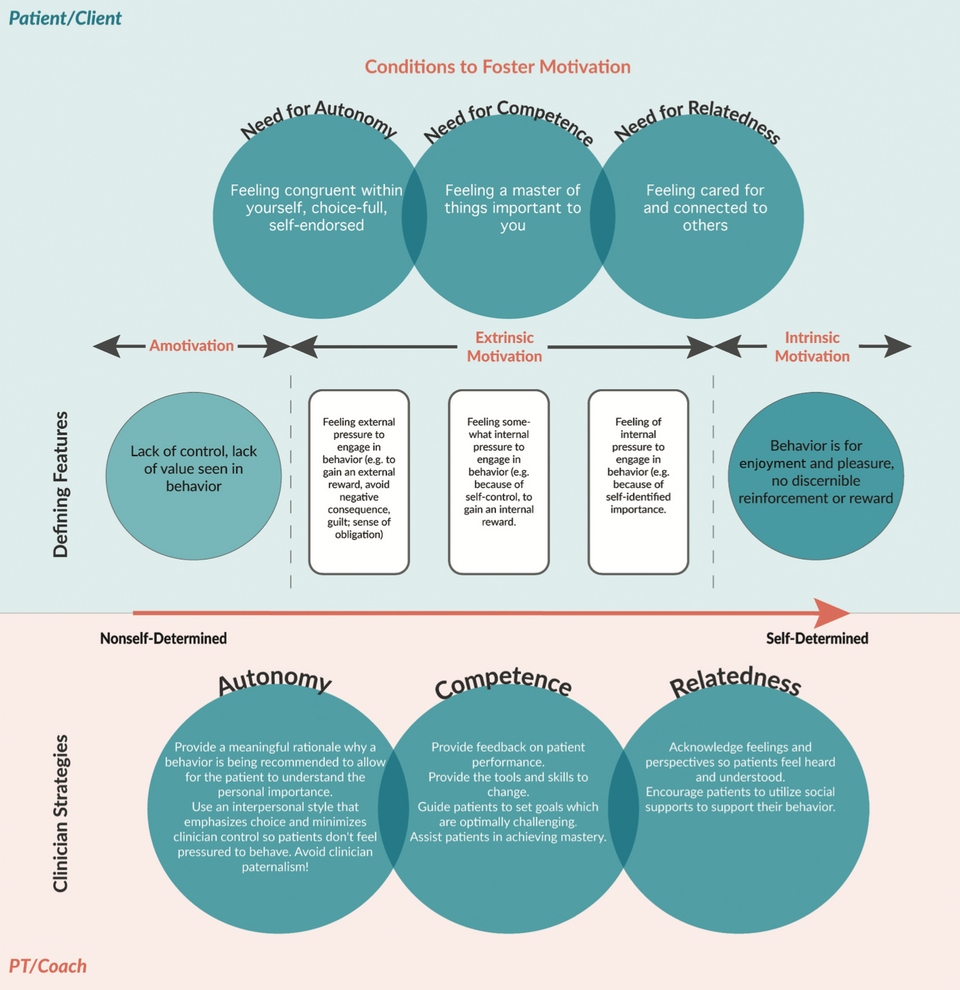
The Gist - In school, pretty much all of us learned about motivational interviewing and we probably practice it and are probably great at it, but this paper argues that doesn’t go far enough. In assessing problems beyond simple PT (like obesity, exercise adherence, unhealthy diets, etc.) these researchers argue that a coach approach is how to not look gauche. In their minds, PTs should adopt a health coaching approach to facilitate behavior change. In this mindset, the PT assumes that the patient is the expert on their body and experiences, rather than the PT. The PTs role is to discover what the patient wants, how they are being held back, and help the patient come up with strategies to achieve this. The PT is a partner, not a leader.
For PTs to successfully change paradigms from expert to coach, three key concepts are useful to understand. First, the patient is the expert of his or her own life. Second, providing education is necessary but not sufficient to catalyze behavior change. Finally, the clinician must have an awareness of when the coach approach and when the expert approach is most effective. Facilitating behavior change is within the scope of practice of a PT and is an important part of the professional role of the PT as even small shifts in individuals’ physical activity, dietary patterns, and stress can result in meaningful reductions in disease burden and cost across populations.
Tell Me More - If you’re interested in how this works functionally, they go on to a case study where they break down ways to change from an expert approach to a coach approach by rephrasing sentences and modifying one’s role. It’s really well laid out and I highly recommend you read it. Afterward, they go deep on theoretical models of behavior change, motivational interviewing, and more, so check those out too if you’re interested, it’s just too much to put here. What I will put here is their discussion of positive psychology, the “scientific study of what makes life worth living.”
In contrast to the typical approach of searching out and defining what is wrong, when facilitating behavior change a clinician can choose to shift attention away from pathology and pain, redirecting it toward a patient’s vision of the good life… It seeks to understand what helps people feel positive emotions and focuses on flourishing doing good out of a sense of purpose or calling. Generating positive emotions and connecting them to an individual’s strengths and vision can be counterintuitive for clinicians trained to identify pathology and problems. It requires they shift from following a “trail of tears” to following a “trail of dreams”.
If you find all of this interesting, do please at least skim the paper. It gets into the weeds on psychology a bit, but most is very understandable for all. PTs are in a great position to health coach because of our relationships with our patients, so do consider this approach if it strikes you as possible.
Paper? Sure thing.
How do you use IASTM?
The Gist - IASTM use is very common and very diverse. That’s the result of this article from the Journal of Athletic Training in which the researchers sent out questionnaires to tons of PTs and ATs to figure out exactly what they’re doing out there. Of the 853 respondents, 83% use IASTM in the practice and 86% of those had some type of formal training. BUT that formal training varied as it was from ten different providers of IASTM tools and the surveyed reported using upwards of 34 different types of tools in practice (total, not each person). Treatment times varied from 1-5 minutes and most of those surveyed (71%) said that they don’t know how to quantify force from their tools.
Tell Me More - Why does all this matter? Because IASTM research can broadly report its practice without getting specific. If we’re all using it differently, it’s tough to quantify what’s really going on. Like the article a few weeks ago that cautioned researchers against using the term “manual therapy” to capture everything from IASTM to cupping to soft tissue massage to manipulations, these researchers point out that using the term IASTM doesn’t capture such a diverse field. In an area where clinicians are using everything from HawkGrips instruments to tongue depressors and butter knives, it’s really tough to get any quantification data on the topic. If you use IASTM in your clinic, it may be time to come up with a protocol and method to test independently, keep track of, and see how it works because we just don’t have that data on an institutional scale yet.
Can you instrument assist me that paper link? Sure, as long as your instrument is a computer.
It’s open access, so here’s your highlighted link to take you right to the stuff you need to know.
And that’s our week, hope you enjoyed it. As usual, I ask that you please share PT Crab with one other person this week to help us keep growing. Any little helps. Bye!
And become a King Crab supporter by subscribing here. The first month is free!






Comments
Want to leave a comment and discuss this with your fellow PTs? Join PT Crab and get summarized PT research in your inbox, every week.