Issue 9 Blue Crab Edition - Why You’re Wrong about Scapulas and IASTM at a Distance
Think You Can Eyeball Scapular Posture? Think Again. Then Measure It Instead.
The Gist - These physiotherapists from Denmark, Australia, and Sweden worked together to see if four PTs could agree on how to rate scapular posture in five different scapular planes under four test conditions. They couldn’t. At least, not very well.
They tested them in the scapular, sagittal, transverse, horizontal, and vertical planes when the subjects were at rest or in one of three different isometric shoulder conditions. Across the 300 ratings from the four PTs, they agreed on neutral 81% of the time (which is great!) but really disagreed anytime they didn’t choose a neutral rating. Generalized kappa was 0.37, indicating low to moderate agreement. So, maybe measure instead of just looking?
Tell Me More - Gladly. In studies like this, you can go really deep into the statistics (if you still remember how they work and haven’t shed every possible memory of EBP from PT school), but I’m not going to. That’s what the whole paper is for. Rather, I’ll note that they did this with 15 volunteers who had chronic mechanical neck pain and gave the PTs normalized criteria with which to rate the scapular positions. They didn’t tell the participants to take any positions intentionally, rather they just had the therapists record the natural position of the scapulas as the tests were performed. Hence the high level of “neutral” ratings.
The authors note that the main problem that led to disagreement may be the uncertainty about what “normal” scapular positions technically are. This leaves things up to interpretation and background, rather than hard data. Hence, measure. Lastly, they don’t know if any of the therapists were wrong or right about their assessments. That wasn’t to point. They just wanted to see if the PTs could agree with one another.
Paper so I can read all the stats? Here it is you nerd.
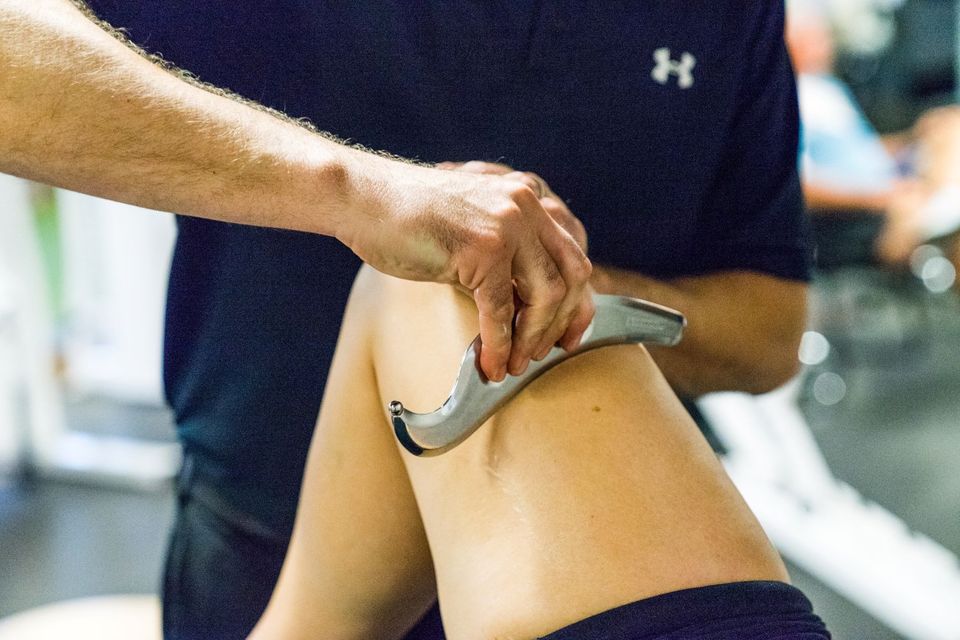
Can you massage one place to improve another? Apparently yes.
The Gist - This week’s first piece of research comes from a familiar journal, as a collection of Greek scientists publish in the Journal of Physical Therapy Science about using Ergon IASTM on the superficial back to improve hamstring flexibility. Huh? Yea, an interesting approach, I know. They targeted the Superficial Back Line of myofascial tissue, applying IASTM strokes down the myofascia of the lateral, upper and mid-thoracic back, and comparing it to similar treatment localized at the thigh and calf, and a third group that received no treatment at all. They used the passive straight leg raise to evaluate hamstring flexibility pre and post treatment, and carried out the treatment once per week for four weeks (except in the control group which got nothing per week for nothing weeks).
Surprisingly, it worked! I mean, you shouldn’t be surprised, because you read the headline of this section, but I was surprised when I read the study. So have some vicarious surprise. 😲. Both experimental groups (leg and back) improved SLR significantly. 6.2% for the back group and 6.6% for the leg. The control group had no improvement (sorry guys 😔).
Tell Me More - Gladly! The genesis of this study (and many others like it) is based on the theory of myofascial chains first published by Thomas Myers in 2001. He studied under Ida Rolf (of Rolfing fame) and developed his theory of the links in myofascial tissue through his studies with her. His scientific chops can feel a bit dubious at times, as they’re largely rooted in alternative medicinal techniques and energy flow. Fortunately, we don’t just have to take his word for it, there is good research (in the Archives of PM&R no less) to demonstrate the veracity of the myofascial chain theory. This study is another step in that very interesting direction.
Back to the research at hand. This research shows positivity about the cumulative effect of IASTM techniques, both locally and distant from a muscle target, and potential myofascial connections that can be utilized in other physical therapy practice as well. What we don’t really know is why these particular spots worked well, beyond the theory of myofascial connections. That could be the reason, but the authors admit that the scientific underpinnings of the theory aren’t completely built out yet. Additionally, this study was limited in its patient population (20-30 year olds with poor hamstring flexibility and no previous injuries) and approach (hamstrings only). It’s more of a first step into a larger world.
Paper? Yupp. Yupp. Yupp.






Comments
Want to leave a comment and discuss this with your fellow PTs? Join PT Crab and get summarized PT research in your inbox, every week.